 As a physician, I rely on my patients and their families to guide me on the focus of care they want to live their best life. However, if a patient hasn’t discussed that care with their loved ones, and becomes unable to share their healthcare wishes with me, how can I honor unexpressed decisions?
As a physician, I rely on my patients and their families to guide me on the focus of care they want to live their best life. However, if a patient hasn’t discussed that care with their loved ones, and becomes unable to share their healthcare wishes with me, how can I honor unexpressed decisions?
Help your family and your care team by taking charge of your healthcare decisions. The first step is to understand your options. In addition to speaking with your physician, the website prepareforyourcare.org offers excellent step-by-step instructions with video and free forms to guide you in your planning.
It’s time to talk
Once you have an idea what your wishes are, it’s time to talk about them. It is hard to start this conversation. So approach it from the perspective that it is an act of love to make your family aware of how you would like to be cared for in the event of a medical emergency, while coping with advanced illness, or at the end of your life. You will be taking the first step of removing the burden these decisions may have for your family, by making these decisions on your own behalf.
The final step is to document these decisions, and in a way that is legally binding. It is important to understand that certain states and jurisdictions require different documentation for certain medical decisions. In the state of Maryland, the documentation physicians look for are advance directives and the Medical Orders for Life Sustaining Treatment form, known as the “MOLST”.
 Advance directive
Advance directive
An advance directive is a legal document that has two parts. One part names a medical proxy or healthcare agent, someone you have selected to make healthcare decisions when you are unable to make those decisions yourself. The other part is the living will, which includes the instructions for your future medical treatment, whether it is future inpatient treatment or end-of-life care. An excellent website to help you create a legal advance directive is fivewishes.org.
MOLST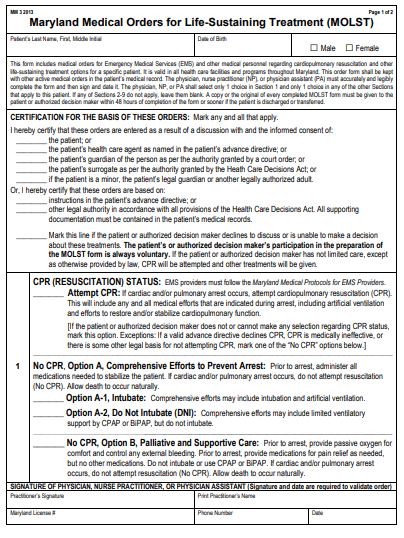
The MOLST form is a set of medical orders that define life-sustaining treatment that a patient wants to receive or avoid. A physician, nurse practitioner or physician’s assistant must complete or change the MOLST based on the patient’s current medical condition, prognosis, values, goals and preferences. If you live in Maryland and you do not want CPR, a MOLST form is the only document first responders and healthcare professionals will follow. You can download a form to share with your primary care team at www.whymolst.com.
If you don’t tell them, how will they know? Take charge of your healthcare: Understand your options, discuss your preferences, document your decisions and advocate for yourself.


